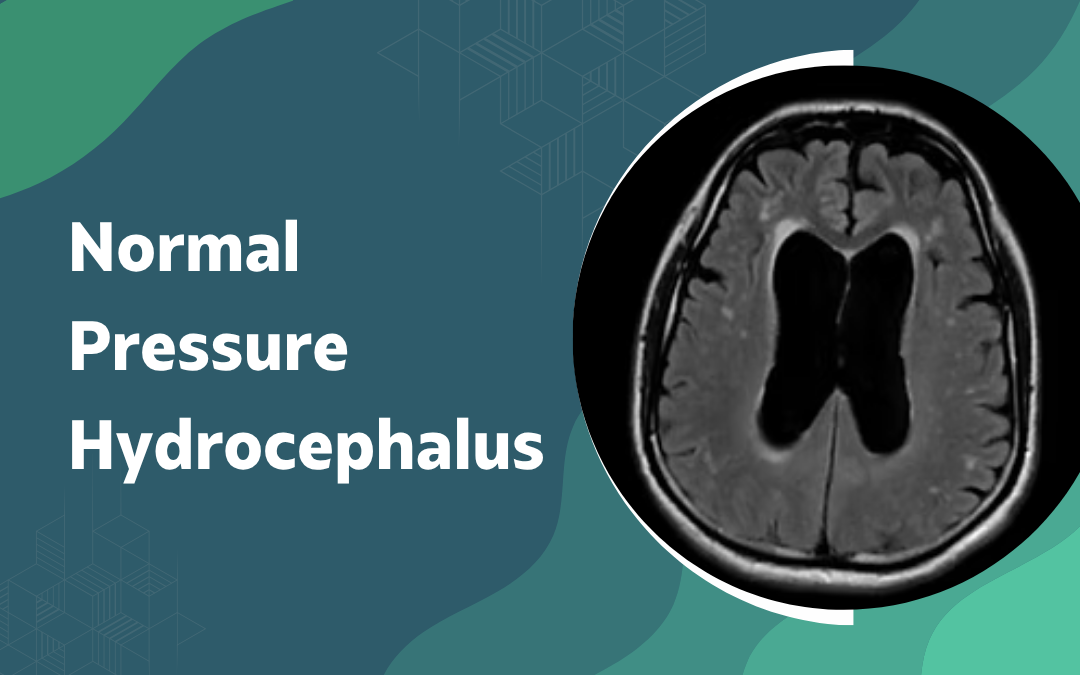
Normal pressure hydrocephalus gets misread as dementia all the time, because the two look so alike from the outside. Memory slipping. A shuffling, unsteady walk. Trouble with the bladder. But here’s the part that matters: NPH is a fluid problem, not a dying-brain problem. Too much cerebrospinal fluid pooling in the ventricles, with the pressure still reading normal. And unlike Alzheimer’s, it’s treatable. A shunt to drain the fluid can turn a lot of it around.
According to Dr. Gurneet Singh Sawhney, a leading Neurosurgeon in Mumbai, this is the diagnosis nobody wants to miss, because it’s one of the only causes of dementia-like decline you can actually reverse. An older person written off as having Alzheimer’s might just have a plumbing problem, and a shunt can hand them years back.
An older relative declining fast with an unsteady walk?
Why Is NPH Mistaken for Dementia?
The symptoms overlap almost completely, so on the surface the two look like the same illness.
Memory: the slowed thinking and forgetfulness read exactly like early Alzheimer’s, which is usually the first wrong label
Walking: a magnetic, shuffling gait, feet that seem glued to the floor, gets blamed on age or Parkinson’s
Bladder: loss of bladder control shows up too, and it’s easy to file under general decline rather than a clue
Age: it hits the same older group as dementia, so nobody’s surprised, and nobody digs deeper
And that’s the tragedy, a treatable condition gets shelved as one that isn’t. Catching it early opens the door to brain surgery that can genuinely turn things around.
How Is NPH Diagnosed and Treated?
The workup is about proving it’s fluid, not degeneration, and then draining the excess.
Scan: an MRI shows ventricles ballooned out of proportion to any shrinkage, the giveaway that fluid, not loss, is the trouble
Tap test: drain some fluid by lumbar puncture, watch the walk improve, and that all but confirms it
Shunt: a thin tube, placed during hydrocephalus treatment, carries the extra fluid away for good
Timing: the earlier it’s caught the more comes back, gait first, then often the memory and the bladder
The clinical priority is identifying a treatable cause before attributing the decline to irreversible neurodegeneration. This overview of Parkinson’s disease outlines the overlapping features that frequently complicate early diagnosis of NPH.
Why Choose Dr. Gurneet Singh Sawhney?
Dr. Gurneet Singh Sawhney trained in neurosurgery in Japan and has more than 18 years placing shunts and separating the treatable causes of decline from the ones that aren’t. With NPH, that distinction is the whole ballgame.
Families walk in braced for a dementia diagnosis and sometimes leave with a fixable one instead. That’s a rare kind of good news. The shunt won’t help every case. But for the ones it fits, watching someone walk steadily again says it all.
Frequently Asked Questions
Can normal pressure hydrocephalus be cured?
It can’t be cured, but a shunt often reverses much of the decline.
How is NPH told apart from dementia?
An MRI and a fluid tap test show it’s fluid, not brain loss.
What are the three main symptoms of NPH?
Trouble walking, memory decline, and loss of bladder control, often together.
Does NPH only affect older people?
Mostly yes, idiopathic NPH is largely a condition of older adults.
Disclaimer: The information shared in this content is for educational purposes only and not for promotional use.