1. Curative Epilepsy Surgery
Curative epilepsy surgeries are performed to remove the seizure focus area without causing damage to the brain or loss of brain function. Curative epilepsy procedures include lobectomy, cortical excision, and hemispherectomy that focus on removal of the area of the brain that causes seizures.
Dr. Gurneet Sawhney, one of the top neurosurgeon in India, may suggest curative procedures only if the diagnostic tests pinpoint the exact origin of the seizure in the brain.
2. Temporal lobectomy
Neurosurgeons perform this surgery on patients suffering from temporal lobe epilepsy. There is a nearly 70% to 80% reduction in the intensity of the seizure or complete control. The patient’s memory and language can be affected if the surgery is performed on the dominant hemisphere.
3. Cortical excision
This surgery focuses on removing the outer layer of the brain at the focal area of the seizure. The cortical excision surgery has promising results with significant improvement in seizure control in nearly 50% of the patients.
4. Hemispherectomy
The neurosurgeon will remove the outer layer and the anterior temporal lobe in one section of the brain. Surgeons perform hemispherectomy on children in most cases. It is performed on patients who suffer from intractable seizures and are weak on one side of the body.
These patients usually have a damaged hemisphere in the brain. Post hemispherectomy, the patients show remarkable improvement in attention span, behaviour, and cognitive functioning.
5. Palliative Epilepsy Surgery
Palliative epilepsy procedures focus on reducing the frequency of seizures and/or their severity. The patients have to undergo in-depth testing to locate the exact source of the seizure and the impact of its removal.
Palliative epilepsy procedures are critical procedures as they could affect the quality of life, especially mobility and speech. Palliative procedures include corpus callosotomy, multiple subpial transections, vagus nerve stimulation (VNS), and deep brain stimulation (DBS).
During the DBS procedure, the surgeon places a pair of electrodes in the brain. The generator that controls it is implanted in the chest. The frequency and its levels are customized as per the patient while the stimulation remains continuous.
7. Corpus callosotomy
This procedure is a preventive surgery that focuses on preventing the spread of generalized seizures from their original location by disconnecting a section of nerve fibres across the corpus callosum. In the first surgery, the front area of the corpus callosum is sectioned. If the patient does not improve, then the rear area of the corpus callosum is treated in the same manner.
There have been instances of the issue in left-right motor coordination, mutism, and apathy in patients who have undergone total corpus callosotomy. This procedure is a curative and preventive procedure done to prevent the spread or the intensity of seizures.
8. Multiple subpial transections
This procedure involves the creation of small incisions in the brain, especially in the seizure focus area, so that they interfere with the spread of the seizure. This procedure is done in combination with lobectomy or alone. Surgeons perform multiple subpial transections in the seizure focus area in the brain’s vital area, which cannot be removed.
9. Vagus Nerve Stimulation (VNS)
In this procedure, the neurosurgeon implants a device that performs functions similar to a heart pacemaker. This device produces electric signals to prevent seizures. The patient can switch on the device indicating the onset of a seizure, and electric signals will be sent to the brain through the vagus nerve.
Neurosurgeons perform VNS on patients who cannot undergo brain surgery. It is not a cure for epilepsy and is not successful in all patients. It can reduce the seizure frequency to about 30%.
The patient could suffer from mild hoarseness in the voice and tingling sensation in the neck in the event of stimulation.

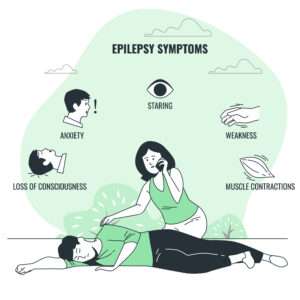 During epilepsy, a person exhibits abnormal behaviour, symptoms, and sensations, including loss of consciousness. Epilepsy has only a few symptoms.
During epilepsy, a person exhibits abnormal behaviour, symptoms, and sensations, including loss of consciousness. Epilepsy has only a few symptoms.





