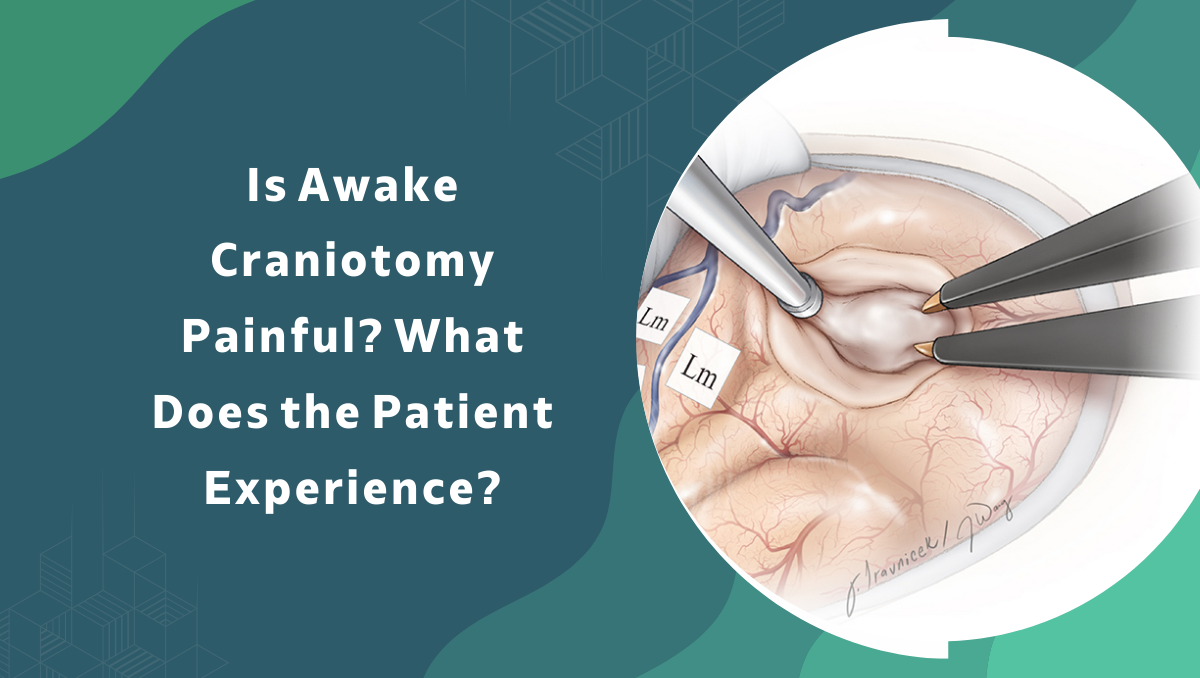
No. It’s not painful. The brain genuinely has no pain receptors not a small number, none. There’s nothing inside the skull that registers a pain signal. And the scalp, which does have receptors, gets numbed with local anaesthetic before the first incision. So what people are actually awake for the mapping, the tasks, the couple of hours of lying still doesn’t involve pain from the surgery. Discomfort from staying in one position, yes. Strangeness, definitely. Pain from what the surgeon is doing, no.
Dr. Gurneet Singh Sawhney is a neurosurgeon at Fortis Hospital Mumbai. He performs awake craniotomy for brain tumors near speech and motor areas. Most patients come in certain it will be unbearable. Most leave saying it wasn’t.
Want to understand what this procedure actually feels like before deciding anything?
What Actually Happens, Start to Finish
Because vague reassurance doesn’t help. Knowing the sequence does.
You’re sedated for the parts that would actually be distressing: Before anything happens before the incision, before the drill, before the bone comes off you’re sedated. Relaxed, not unconscious, but not tracking what’s happening either. Local anaesthetic has already gone into your scalp. The neuroanesthesiologist running this phase isn’t working from a standard general anaesthesia protocol. Awake craniotomy has its own sedation approach. By the time sedation lifts, the skull is already open. People researching brain tumor surgery in Mumbai consistently find this part surprising — the most frightening-sounding moment is the one you’re not present for.
The awake phase is genuinely strange but not what you’re imagining: Sedation comes down. You wake up. Your head is fixed in a frame that’s uncomfortable the way a long flight is uncomfortable, not painful. There’s pressure. A sense that things are happening nearby. But the surgical site isn’t sending pain signals because it can’t. What’s actually happening is a neuropsychologist beside you, going through tasks. Name the object on the card. Count down from a hundred. Move your fingers. Over and over. Some patients find it meditative. A few fall asleep mid-task. Families who’ve read about whether neurological problems can exist with normal scans usually arrive already understanding why the live feedback from tasks matters more than anything imaging can show.
Anxiety is expected and managed you don’t have to white-knuckle it: The neuroanesthesiologist doesn’t leave the room. If things get distressing genuinely distressing, past nervous into something harder sedation goes up immediately. This isn’t a procedure that needs the patient to be brave. It needs the patient to be functional enough to complete the tasks. There’s a difference. Once mapping and resection are done, sedation returns for the closure. You wake up in recovery. It’s finished.
The Part Most People Get Wrong About Awake Surgery
The fear isn’t wrong. It’s just aimed at the wrong part of the procedure.
Understanding what happens reduces anxiety more than anything else: Patients who go in knowing the sequence what sedation feels like going down, what pressure awareness feels like, what the tasks actually involve consistently report less distress during the procedure than patients with gaps in that picture. The pre-surgical briefing exists for exactly this reason. Not as box-ticking. Because it works.
Some patients aren’t suitable and that’s assessed beforehand: Severe claustrophobia. Anxiety that doesn’t settle with preparation. Cognitive difficulty following task instructions. All of this gets assessed before surgery is scheduled. The pre-surgical evaluation isn’t just about whether awake craniotomy is surgically indicated it’s about whether this specific patient can do it comfortably. Both questions get answered before anyone commits to anything.
As a Neurosurgeon in Mumbai who does this regularly, Dr. Sawhney’s pre-surgical consultation leaves no gaps. Patients know exactly what they’re walking into. And what they walk into is consistently less frightening than what they imagined.
Why Choose Dr. Gurneet Singh Sawhney
The surgical side of awake craniotomy requires subspecialty training. But the two hours the patient spends awake depend on something else entirely preparation, the anaesthesia protocol, and who’s actually in the room.
Dr. Sawhney trained under Prof. Taira at Tokyo Women’s Medical University for functional neurosurgery. Then under Prof. Sugano at Juntendo University for epilepsy surgery. Not general neurosurgery with occasional complex cases. Subspecialty training at centres doing this at volume. Back at Fortis Hospital Mulund West, the awake craniotomy team includes a dedicated neuroanesthesiologist and neuropsychologist who work this protocol regularly not put together differently each case. Patients come in scared. They leave having had an experience that was, by their own account, far more manageable than they expected going in.
FAQ's
Does awake brain surgery hurt?
No the brain has no pain receptors and the scalp is numbed before any incision, so the awake phase involves pressure and positional discomfort, not pain from the surgical site.
What does it feel like to be awake during brain surgery?
Strange more than distressing pressure awareness, repeated tasks with a neuropsychologist, and an experience most patients describe as significantly less frightening than they expected beforehand.
What if I panic during the awake craniotomy?
The neuroanesthesiologist is in the room throughout and increases sedation immediately if needed cooperation is required, stoicism isn’t.
How long is the awake phase?
One to two hours for most cases the skull opening and closure both happen under sedation on either side of that window.
How do I consult Dr. Gurneet Singh Sawhney about awake craniotomy?
Call +91 8104310753 or email gurneetsawhney@gmail.com he reviews imaging before the consultation at Fortis Hospital, Mulund West, Mumbai.
References
- National Institute of Neurological Disorders and Stroke. Neurological Diagnostic Tests and Procedures. NINDS, NIH.
- Doraiswamy S, et al. Use of Digital Technologies in Facilitating Healthcare Access. PubMed Central, NCBI.
